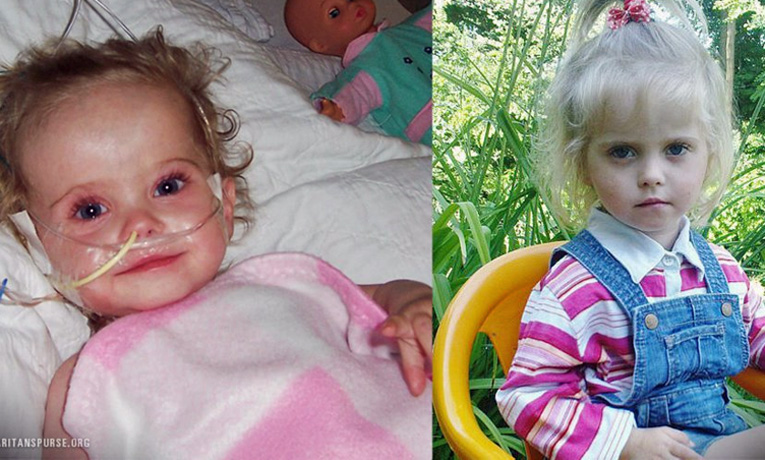
A Children’s Heart Project “miracle child” is a reminder of how God is using the program to save lives—and why more support is needed
Debi Lammert is an Advanced Practice Nurse from Tulsa, Oklahoma, specializing in Pediatrics and Pediatric Surgery/Cardiology/Cardiac Surgery, and a long-time volunteer with Children’s Heart Project. During Congenital Heart Defect Awareness Week, she writes about a memorable girl from the early years of the program.
“Her name is Azra,” her mom whispered, glancing at me shyly as the translator related the information. She then looked around carefully, afraid that the nurses or doctors in the Sarajevo Hospital’s Pediatric Intensive Care Unit would hear her words and mock or laugh at her.
Mock and laugh—because why would you name a baby that had almost no chance to live?
GiveAzra’s parents had already made the difficult choice to try to save the life of their firstborn, from the time the doctor handed the blue infant to her father at a hospital outside of war-torn Sarajevo.“Drive her to Sarajevo, as fast as you can,” the doctor said. “If she is still alive when you get there, they might be able to help her.” The words haunted him as he made the desperate two-hour journey alone with his critically ill infant daughter.
Barely alive upon arrival to the hospital, she was placed on oxygen and a limited heart ultrasound was performed. The diagnosis was Transposition of the Great Arteries (TGA), a severe congenital heart defect. A hole between the upper chambers of her heart was letting just enough blood mix together to keep her alive.
The hospital found some expired medicine that would help keep her going a little bit longer, but she would die quickly without it.
Most infants with TGA undergo highly specialized, corrective cardiac surgery within the first two weeks of life. This gives them the best chance at survival, a 95 percent or greater success rate in most developed countries. But the surgery was not available in Bosnia.
While working in Bosnia in 1997, Samaritan’s Purse found many children suffering from congenital heart defects who could not be adequately treated because the country’s ethnic war had damaged hospitals and equipment and forced many doctors to flee. We launched Children’s Heart Project that year to bring boys and girls to North America for life-saving surgery. Azra was one of the first 30 children accepted into the program.
She was 31 days old by the time I was sent as a volunteer transport nurse to bring her to the United States. The hole between the upper chambers was closing, she had a bloodstream infection, and the hospital had one vial left of the lifesaving medicine that had been donated for several weeks by a compassionate doctor from the nearby UN hospital. Azra was a bluish-gray color and was too weak to suck. Her oxygen levels were dismally low.
Standing at the window of the hospital, calling for further advice from a pediatric cardiologist back home, I saw the NATO bombers overhead, using the Bosnian airspace as their flight path to Serbia. The Sarajevo airport was closed.
Several days after arrival and revision of departure plans, we left by “ambulance” (a van with nothing but a stretcher and oxygen) for the six-hour drive to Split on the Croatian coast. Three other Children’s Heart Project children and their mothers were with us, two groups of children destined for charity care in the United States.
After a night in Split, we flew to Vienna. That night, she worsened. Her mother slept in a bed in the room next door with the translator, while I stayed up tending to Azra. The next morning, a Sunday, we got on a plane to America. The final destination was Detroit.
Azra’s mother was worried as we boarded the flight. So was I. She required full IV fluids now, an increase in oxygen and in the special meds, and additional antibiotic therapy for fever. As we got midway over the Atlantic Ocean at 34,000 feet, her breathing became more labored and she became even more lethargic and cyanotic (blue).
In consultation with the Samaritan’s Purse staff member traveling with us, I made the difficult call. “We aren’t going to make it to Detroit; we must land at a capable center in the U.S., as soon as possible.”
Phone calls were made from the airplane, and soon a miracle began to unfold. A key person had missed her early church service, and was home to take our call. She had cardiology connections in Atlanta.
A pediatric cardiologist at a highly respected children’s hospital agreed to care for Azra. He would meet us on the tarmac with the mobile Intensive Care Unit and staff. The pilot was notified and altered the flight pattern to get us to Atlanta more quickly.
We prayed and knew that others on the ground were praying. Azra’s mother clung to the translator’s hand, with a facial expression that was at the same time both terrified and resigned.
This rapidly deteriorating infant was quickly whisked away to the hospital upon landing and immediately taken to the Cardiac ICU. Within 20 minutes of arrival, she was in the heart catheterization lab and stabilized. She had her first surgery three days later, and four weeks later her second.
Eight weeks after her dramatic arrival in the U.S., Azra and her mom returned home. Nurses, surgeons, various hospital personnel, host families, church members, even media representatives who now considered themselves friends were there for the sendoff.
I was able to fly to Atlanta to say goodbye, and to present Azra’s mother with a very special homemade photo album entitled, “Azra’s Long Journey.” It featured a once blue and almost lifeless—and now pink, alert, playful, and very much alive—little baby name Azra. A true and living miracle!
Over the years, I have been honored to provide medical escort services to over 80 children for the Samaritan’s Purse Children’s Heart Project. Most transports are not as dramatic, but all are life changing for the children, their families, communities, host families, and all involved. The impact is far-reaching!
On almost every flight, I have the opportunity to share with fellow airplane passengers about the project, and more importantly that Christ’s love and compassion for these little children is what compels us to do this specialized work.
Sometimes I get on a flight and think, “Why am I doing this?” Friends and relatives think I am crazy for flying to Mongolia, or Uganda, or Honduras, or Bolivia, only to spend one or two nights, and return to the U.S. or Canada.
And then I watch a once-sickly, now-healthy child return to their distant homeland and be swept up into the grateful arms of his or her father. Or I see the groups of Mongolian and Ugandan children and adults accept Christ and be discipled at Heart Camp. Or I visit Bosnia, and see a child like Azra—now a beautiful young teenager—and hear her mother say, “Jesus healed my little girl.”
Not enough children get this opportunity. The waiting lists in each country are long. Too long.
It takes Christ’s love, and people who unselfishly give of their time, money, hospitality, prayers, and love, to make the lists shorter.
There are more miracles waiting to happen.